MOJ
eISSN: 2374-6939


Research Article Volume 13 Issue 4
1National Medical Research Center of Traumatology and Orthopedics named after Academician G.A. Ilizarov “of the Ministry of Health of the Russian Federation, Kurgan, Russia
2Federal State Budgetary Educational Institution of Higher Education “Tyumen State Medical University” of the Ministry of Health of the Russian Federation (FSBEI HE Tyumen State Medical University of the Ministry of Health of Russia)
3Bari-Ilizarov Orthopaedic Centre, Dhaka, Bangladesh
Correspondence: Bari MM, Bari-Ilizarov Orthopaedic Centre, 1/1, Suvastu Shirazi Square, Lalmatia Block E, Dhaka-1207, Bangladesh, Tel +8801819211595
Received: July 30, 2021 | Published: August 13, 2021
Citation: Botasheva AS, Shikhaleva NG, Novikov KI, et al. Questions of the current state of treatment of post-traumatic deformity of the distal radial metaepiphysis. MOJ Orthop Rheumatol. 2021;13(4):85-88. DOI: 10.15406/mojor.2021.13.00554
Based on the analysis of modern scientific Russian and foreign literature, this article includes information about the current state of the treatment of post-traumatic deformity of the distal metaepiphysis of the radius. The statistical information on the number of registered cases with this pathology, gender characteristics of injury, as well as some of the diagnostic radiological aspects is briefly considered.
Keywords: deformities of the distal metaepiphysis of the radius, post-traumatic deformity, traumatization
Anatomically, the distal part of the radius is presented as an irregularly shaped figure, an important role of which is the formation of the wrist and radioulnar joints. An incorrectly chosen algorithm for conservative treatment of fractures of the distal metaepiphysis (DM) of the radius, errors in the choice of tactics for surgical treatment of fresh injuries lead to the formation of post-traumatic deformities.1
The fracture of the distal radius was first described in 1814, but for a long time it remained a poorly understood and complex phenomenon in the orthopedic community.2 Modern scientific withStatistical data show that the unfavorable outcome of the treatment of forearm injuries varies from 13 to 66% and is expressed by the occurrence of pathological formations such as pseudoarthrosis, bone deformities, etc,3–7 a wide range of complications can be associated with the lack of a single algorithm for the provision of medical care. The age indicators of people who have received this type of injury can be divided into two large groups, according to the characteristics of frequency, namely: from 40 to 60 years old - 51%, over 60 years old - 43%.8 It should be noted that both age categories are included in the definition of able-bodied citizens, therefore, a fracture of the distal metaepiphysis of the radius carries complex medical and social consequences and requires careful research and development. Getting injured at a young age is most often due to extreme sports or high-energy loads, while at an older age, injuries occur as a result of falling, for example, from a height.9–11 There is a difference in the gender characteristics of trauma, for example: women have an increased risk of a fracture of the distal metaepiphysis of the radius after 50 years, and by the age of 80, the peak of this type of trauma is reached.12 This was noted on the materials of the study of Norwegian scientists, which are also confirmed by other works.13–16 Thus, the relevance of the topic under consideration is undeniable and important in the context of the listed factors.
The literature review includes publications from open Internet resources, namely: Cochrane Library, PubMed, eLIBRARY, release dates are 1997 and 2019. The selection of articles was carried out by the method of content analysis. Also, general scientific methods were used, such as analysis, comparison, generalization, classification, and the principles of objectivity, consistency, integrity.
Incorrectly healed DMLK fractures significantly impair the patient's quality of life, which leads to the need for surgical treatment. Let us dwell in more detail on the clinical picture and the functional state of the patient.
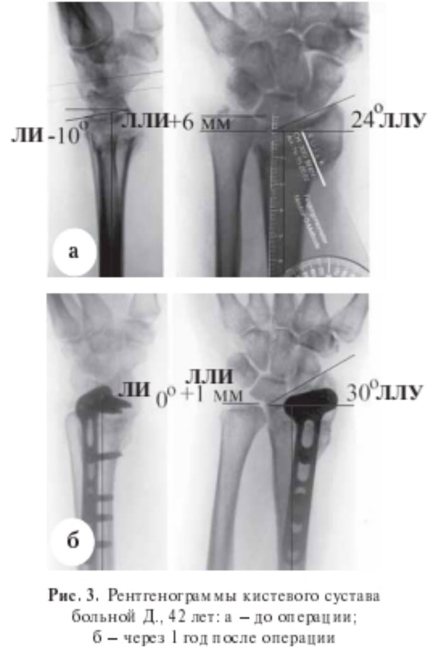
Figure 1 Radiographs of the wrist joint of patient D., 42 years old, a - before the operation; B - one year after the operation.17
Treatment of post-traumatic deformity of DMLK is of two types: conservative and operative. Mulders M., considering the results of his practice, is convinced that the effectiveness of both surgical and conservative treatment is on an equal level.24 Recently introduced internal fixation devices have provided hand surgeons with additional options for treating intra-articular fractures of the distal radius. However, modern technologies of X-ray examinations and surgical support, as well as the availability of new means of bone osteosynthesis, are the impetus for surgical operations that improve the quality of life. This process is common to orthopedic traumatologists around the world.25 However, visualization of the articular surface of the distal radius after the plate has been applied can be difficult on standard straight and lateral radiographs due to the location of the plate directly below the articular surface. Although several studies of cadaveric material have shown that angular radiographs can better demonstrate the articular surface. No study comparing the efficacy of standard straight and lateral distal radial images with angular radiographs for evaluating fixation devices dorsally placed on the distal radius has not been performed.26 Thus, improperly fused DMLK fractures lead to a number of negative consequences for the functioning of the hand, wrist, and radioulnar joints. The lack of surgical treatment will lead to irreversible consequences, however, an important role is played by rehabilitation measures, which allow preventing the development of contractures, edema, and neurodystrophic syndromes. Alsothe presence of an intra-articular fracture of the distal joint can lead to the development of premature arthritis of the wrist, elbow and distal wrist joints. Numerous studies have shown that residual articular deformity of 1-2 mm during fracture healing, attributed to signs of arthrosis according to X-ray studies, leads to negative results.27 On the contrary, in additional studies,28,29 concluded that symptomatic arthritis is rare after intra-articular fractures of the distal radius, despite radiological signs of arthrosis. Since each of these studies has shown that persistent residual joint misalignment at the time of fracture connection leads to radiological signs of premature arthrosis (but not necessarily arthritis), it seems reasonable that the treating surgeon should achieve as close anatomical fusion as possible in order to minimize the development of early degenerative changes. Accurate assessment of the distal radial articular surface (pre-reduction and post-reduction) requires careful radiographic evaluation.
The existing progress in medical science allows us to revise the established views on the issue of DMLK treatment, suggesting the use of technically improved equipment, other methodological aspects at the preoperative stage of working with a patient, and much more. However, it should be noted that, despite all of the above, the use of external osteosynthesis, despite its popularity, does not solve the issues of minor post-traumatic deformity (1-2 mm), which causes osteoarthritis and arthritis of the affected segment, and also complicates the X-ray observation of DMLK and postpones the start of rehabilitation measures. Thus, the use of transosseous osteosynthesis according to Ilizarov has a number of immediate advantages (Figure 2 & 3).
None.
The authors declare no conflicts of interest.

©2021 Botasheva, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.