eISSN: 2378-3176


Research Article Volume 14 Issue 1
Consultant Urological Surgeon, Department of Urology, University Hospital of North Tees and Hartlepool, NHS Foundation Trust, United Kingdom
Correspondence: Ashwini Gaur, MB.BS (Delhi), F.MAS, CCST (Urology) Moldova, FEBU, FRCS (Urol), DLS (Strasbourg), Consultant Urological Surgeon, Department of Urology, University Hospital of North Tees and Hartlepool NHS Foundation Trust, Stockton on Tees, TS19 8PE, United Kingdom., Tel 07501290721
Received: March 12, 2026 | Published: March 30, 2026
Citation: Gaur A. Hyoscine butylbromide at induction enables pre-stent-equivalent renal access in Retrograde Intrarenal Surgery, cutting costs and reducing stent duration. A single surgeon, single center comparative cohort audit. Urol Nephrol Open Access J. 2026;14(1):21-25 DOI: 10.15406/unoaj.2026.14.00367
Background/objectives: Renal access remains a limiting factor in Retrograde Intrarenal Surgery (RIRS), particularly in non pre- stented patients. Hyoscine butylbromide (Hbb) is an antispasmodic agent which has not been studied in RIRS. This study evaluates role of intravenous Hbb at induction for facilitating renal access in non-pre-stented RIRS patients, benchmarking outcomes against pre-stented patients.
Methods: Retrospective analysis of prospectively maintained data from 360 RIRS procedures (Jan 2018-Dec 2024). Patients were divided into two groups: Group A (non-pre-stented + intravenous Hbb at induction, n=151), Group B (pre-stented, no Hbb, n=209). Men on Tamsulosin were excluded in group A (n=15). Outcomes included failed renal access, ureteric injury, stent duration and strictures.
Results: Failed kidney access: Group A 3.9% and Group B 1.9% (A and B, p=0.33). Ureteric injury was observed in 10.59% and 5.3% in Groups A and B, respectively (A vs B, p=0.069). Mean stent duration in group A and B was 18 ± 11.4 and 49.01 ± 9.5 days, respectively (p<0.05). One ureteric stricture occurred in each group.
Conclusions: Intravenous Hyoscine butylbromide at induction in non-pre-stented patients achieves renal access rates comparable to pre- stented RIRS patients, with shorter stent duration, reducing National Health Service costs from additional procedures and improving QoL by minimizing stent symptoms-a safe single session alternative.
Keywords: retrograde intrarenal surgery, hyoscine butylbromide, ureteral access sheath, flexible ureterorenoscopy, ureteric stricture, ureteric injury, renal access
Retrograde intrarenal surgery (RIRS) or flexible ureterorenosocopy (f-URNS) has become a mainstay in the management of renal calculi. Renal access remains a limiting factor, particularly in non-pre-stented patients, where success rates are reported as low as 58.8%.1
Hyoscine butylbromide (Hbb) IV is licensed for acute spasm, explicitly including renal or biliary colic and spasms in radiology/procedures (e.g., pyelography, endoscopy where spasm obstructs).2,3
Pre-stenting patients results in an increased number of procedures, cost, and poor quality of life due to stent symptoms.4,5 Ureteral access sheaths (UAS) can facilitate repeated entries with f-urns and improve visualization by improving drainage from the kidney, but their use can result in complications like ureteric injury and, ureteric strictures.6,7
Pharmacological agents like alpha-blockers have been studied to improve the ureteric access rates.8,9 However, overall ureteric injury rates are still high compared to pre-stented patients.9 Hbb is a quaternary ammonium anticholinergic that relaxes smooth muscle through muscarinic M3 receptor blockade. It is commonly used in gastrointestinal endoscopy to facilitate scope passage and mucosal visualization,10-12 but its role in endourology is unexplored. With regard to its safety profile, parenteral administration of Hbb is associated with mild and self-limiting adverse events, typical for anticholinergic drugs.8 Hbb is a very commonly used drug across the world. It is commonly given in the emergency or ward as i/v injection. There is no published data on use of Hbb in RIRS.
This study evaluates intravenous Hbb at induction for renal access in non-pre-stented RIRS patients, benchmarking outcomes against pre-stented patients.
Study design
Retrospective analysis of a prospectively maintained RIRS audit database (Audit no. 2579) performed in a single NHS Trust.
Ethics approval and informed consent
This study was done as an extended arm of an already approved audit no. 2579. No formal ethical approval was sought as this reports routine clinical practice using Hbb within licensed indications for acute spasms, including renal colic and spasms in procedures (eg. pyelography).2,3 It meets the definition of clinical service evaluation per HRA Decision Tool (UK) and local policy- no systematic research or new interventions were introduced. All data were fully anonymized; patients provided written generic surgical consent.
Population
Between January 2018 and December 2024 Three Hundred and Sixty consecutive patients met the inclusion criteria. Mean age was 59.6 ± 15.8 years (range 21- 89); 187 males, 173 females. Patients with significant cardiac comorbidities, acute angle closure glaucoma, and myasthenia gravis were excluded due to the anticholinergic side effects of Hbb.
Study groups
Group A: Inclusion: Non-pre-stented patients who had intravenous Hbb 10-20 mg at induction and were not on alpha bockers (n=151; 66 males, 85 females); all operated by the author.
Exclusion: Men who were on alpha blockers for LUTS were excluded (n=15).
Group B: Inclusion: Pre-stented patients who did not receive any Hbb (n=209; 119 males, 90 females). These patients had stent inserted for obstructive ureteric stones in emergency and also had renal stones or proximal ureteric stones that migrated to the kidney during the stenting and were booked electively for staged rigid and flexible ureterorenoscopy and laser treatment post-stenting; all operated by the author. The stent was present in these patients prior to the second procedure or staged RIRS for atleast 6 weeks due to waiting time in UK NHS.
Sample size determination
This study utilized a retrospective convenience sample including all 360 consecutive RIRS procedures performed during the study period (January 2018 to December 2024) that met the inclusion criteria (Group A: non-pre-stented + Hbb, n=151; Group B: pre-stented no Hbb, n=209). Total analyzable cohort: n= 360.
Post-hoc power analysis (two- sided α=0.05, proportion test).
Failed renal access: 3.9% A vs 1.9% B shows 21% power. For ureteric injury (10.5% vs 5.3%), power is 47%. These modest powers reflect small observed absolute differences and support exploratory equivalence benchmarking against pre- stenting. RCT confirmation warranted.
Definitions
Failed renal access was defined as inability to advance the flexible ureterorenoscope (F-URS) into the kidney due to tight proximal ureter in spite of successful placement of the guide wire and ureteric access sheath till mid/proximal ureter.
Ureteric Access Sheath (UAS) not passable was defined as a ureteric access sheath that could not be advanced in the ureter or beyond the distal ureter, but F-URS passed successfully in the kidney.
Stent Duration: For Group A, stent duration is defined as the duration the stent stayed in following the RIRS or, in case of failed access the duration the stent stayed in following the 1st failed access until the patient was stent free post RIRS.
In group B the stent duration was calculated from the day the stent was first placed in emergency for ureteric colic for the staged procedure until the patient was stent free post RIRS.
Ureteric Injury: Defined as injury to the ureteric mucosa or submucosal injury or perforation graded using the PULS13 (Post ureteroscopic lesion scale) score, Grade 0: No lesion, Grade 1: only superficial mucosal lesion and/or significant mucosal edema or hematoma, Grade 2: Submucosal lesion, Grade 3: Perforation with less than 50% partial transaction, Grade 4: More than 50% partial transaction, and Grade 5: Complete ureteric transaction.
Surgical procedure
Standardized technique was used: sensor-tip guide wire, 11/13 Fr ureteral access sheath (36 cm in females and 46 cm in males), imaging intensifier, 8.4 Fr digital f-URS, and JJ stents (5-6 Fr multicoil stents or 6 Fr x 26 cm magnetic stent). An access sheath was passed over the sensor-tip guide wire under X-ray guidance. Successful UAS placement was considered if it could be advanced in or beyond the mid ureter with ease to allow multiple access. In group B, all patients prior to access sheath placement or f-URS also had rigid ureteroscopy. In group A, the ureter was calibrated with the inner dilator of the UAS before insertion of the UAS.
Anesthetic: General anesthetic (GA) with paralysis was used for most patients, and a spinal anesthetic was used in patients not fit for a GA. Hyoscine butyl bromide 10- 20 mg i/v was administered by the anesthetist at induction, 10 minutes prior to starting the procedure. If there was no or mild tachycardia after giving 10 mg Hbb further 10 mg was administered, otherwise, only 10 mg Hbb was given. Prophylactic Antibiotics were administered prior to starting the procedure.
Primary and secondary outcomes
Primary outcomes included failed kidney access and ureteric injury. Secondary outcomes included stent duration and ureteric strictures.
Follow up: Ultrasound of Kidneys, Ureter and Bladder or Non Contrast Computed Tomography (NCCT) scan 4- 6 weeks post stent removal. The hospital's online clinical portal was checked until November 2025 to make sure there was no admission with stricture.
Statistical analysis
All statistical analyses were performed using IBM SPSS Statistics (Version 29.0, IBM Corp., Armonk, NY, USA). Categorical outcomes (Failed access, UAS not passable, Mucosal erosion): Fisher's Exact Test was applied when expected cell counts were <5; otherwise, a two-proportion z-test was used for approximate p-values and 95% confidence intervals for relative risk (RR). Continuous variable (Post-operative stent duration): Welch's t-test was used to account for unequal variances between groups. Mean difference (MD) and 95% confidence intervals were computed accordingly. Effect sizes were calculated where appropriate to quantify the magnitude of differences. All hypothesis testing was two-tailed with p<0.05 considered statistically significant.
Data availability
The author confirms the availability of and access to all original data reported in this study. Anonymized data underlying this study are available from the corresponding author on reasonable request, subject to approval by the NHS Trust Research Ethics Committee and compliance with data protection regulations (UK Data Protection Act 2018 and UK General Data Protection Regulation). Requests for data access should be directed to the corresponding author with appropriate institutional affiliation and research justification.
Baseline characteristics
Transient tachycardia was noted following administration of intravenous Hbb at induction, which resolved promptly intraoperatively without any adverse effect.
Pairwise statistical comparisons can be seen in Table 1
|
Outcome |
Comparison |
n (A/B) |
Group A (%) or Mean ± SD |
Comparison Group (%) or Mean ± SD |
Measure |
95% CI |
p-value |
|
Failed kidney access |
A vs B |
151 / 209 |
3.90% |
1.9% |
RR = 1.89 |
0.47 -- 7.53 |
p=0.33 |
|
Ureteric Injury |
A vs B |
151 / 209 |
10.59% |
5.3% |
RR = 1.98 |
0.91 -- 3.60 |
p=0.069 |
|
Mean stent duration (days) |
A vs B |
151 / 209 |
18 ± 11.4 |
49.01 ± 9.5 |
MD = −31.0 days |
−33.2 to -- 22.8 |
P=<0.05 |
Table 1 Pairwise statistical comparison between groups A and B
Abbreviations: RR, relative risk; MD, mean difference; D, days
*p<0.05 (statistically significant), p>0.05(NS, not significant). Group A: non-pre-stented + IV Hbb (n=151); group B: pre-stented, no Hbb (n=209). Fisher's exact test was used for categorical variables. Welch's t-test for continuous variables.
Access Outcomes
Failed kidney access with flexible ureterorenoscope even if UAS was advanced till mid ureter or proximal ureter occurred in Group A 6/151 (3.9%; 95% CI -7.7). Group B had 4/209 (1.9%) failed access, all 4 of which needed full-length balloon dilatation due to very tight ureter (Figure 1).
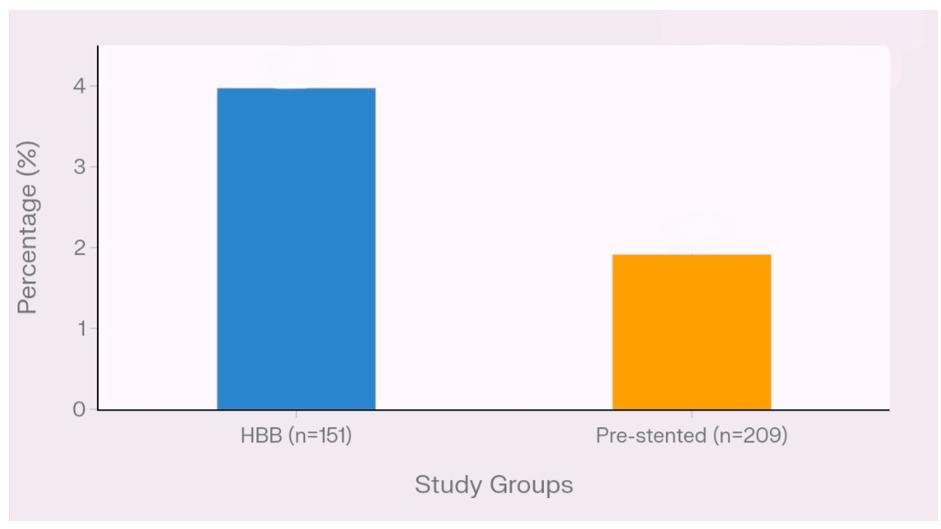
Figure 1 Failed renal access across study groups. Bar chart displaying the percentage of failed kidney access in the two study groups. Group A (non-pre-stented + IV Hyoscine butyl bromide (Hbb) at induction) demonstrated a failed access rate of 3.9% (6/151 patients, 95% ci 1.3-7.7). Group B (pre-stented, no Hbb) showed a failed access rate of 1.9% (4/209 patients). No significant difference was observed between groups A and B (p=0.33, RR=1.89).
Pairwise comparisons and clinical significance
A vs B (Hbb vs Pre-stented): Comparable failed renal access rates (3.9% vs 1.9%; RR 1.89,95% CI 0.47-7.53, P>0.05), with no significant difference. Ureteric injury was similar (10.59% vs 5.3%; RR 1.98, 95% CI 0.91- 3.60, p>0.05). These findings demonstrate Hbb enables access akin to pre-stenting, avoiding staged procedures.
UAS was not passable in 2/151(1.3%) in Group A and while in group B it was passable in all; however, 4 (1.9%) of 209 patients in B required full length ureteric balloon dilatation to successfully pass the access sheath. P>0.05. In 145/151 (96.02%) patients in group A, the access sheath was placed until below PUJ or proximal ureter, and in 4 until mid ureter.
Ureteric injury
Ureteric injury was observed in, (16/151)10.59% patients in group A, of which 3.9% were grade 1 and 6.6% were grade 2 or 3 based on PULS score[9]. In group B (11/209), 5.26% had ureteric injury, of which 2.3% had grade 1 and 2.8% had grade 2 or 3 (p>0.05) (Figure 2).
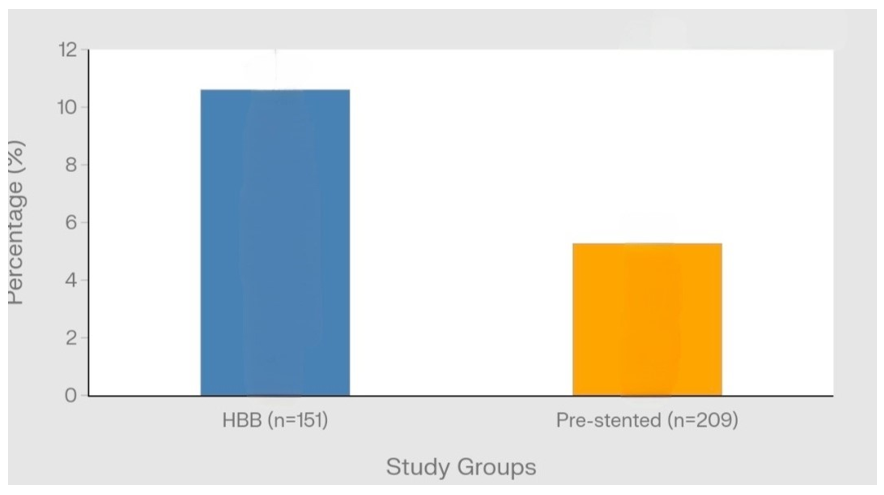
Figure 2 Ureteric injury rates across study groups. Bar chart showing ureteric injury rates in the two study groups. Group A (Hbb group) demonstrated a ureteric injury rate of 10.5% (16/151 patients). Group B (pre-stented group) showed a ureteric injury rate of 5.3% (11/209 patients). Comparison group A and B (p> 0.05).
Ureteric strictures
One ureteric stricture occurred in each group.
Stent duration
Mean stent duration was much less in Group A compared to B and differed due to pre- stenting in B (18±11.4 vs 49.01±9.5 days; MD-31 days, p<0.05), though post- RIRS duration in B was 13.3±9.2 days (Figure 3).
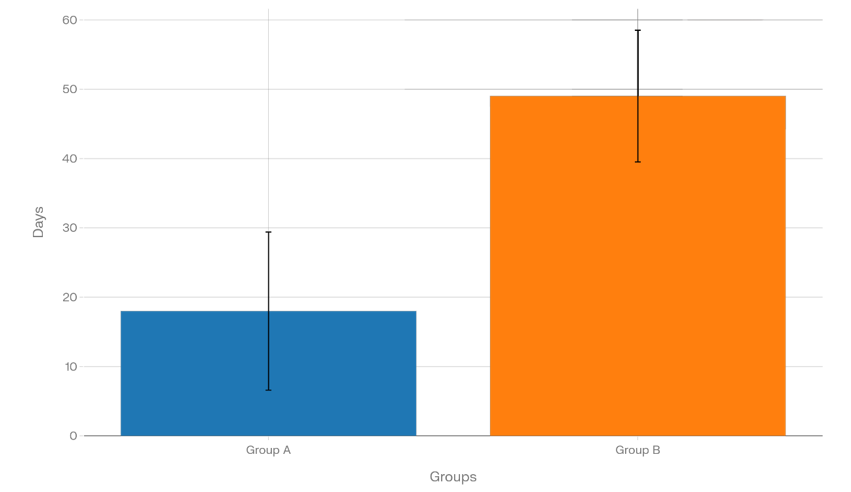
Figure 3 Stent duration across study groups. Bar chart displaying mean stent duration (days) with standard deviation for the two study groups. Group A (Hbb group) had a mean stent duration of 18 +/- 11.4 days (n=151). Group B (pre-stented group) had the longest mean stent duration of 49.01+/- 9.5 days (n=209) due to pre stenting. Welch's t-test revealed statistically significant differences: comparison between groups A and B showed group A had shortest stent duration (p<0.05, MD = −31.0 days, 95% CI −33.2 to -- 28.8 days).
This study provides the first evidence that intravenous Hyoscine butyl bromide (Hbb) at induction significantly improves renal access in RIRS and reduces stent duration, in non-pre-stented patients, therefore reducing the need for staged procedures and improving the quality of life of the patients.
Pre-stented ureters offer improved access for retrograde intrarenal surgery;1,4,5 however, this comes with significant stent symptoms and the need for an additional procedure or anaesthetic to insert a stent prior to stone removal, this which adds to additional costs to NHS and inconvenience to the patients, affecting QoL. In this study, the pre-stented group had their stent placed for obstructive ureteric stone in an emergency (not electively), and also had renal stones on the same side. These patients typically waited for at least 6 weeks before undergoing a procedure for stone removal, a waiting time consistent throughout the UK NHS for staged procedures.
Pairwise comparisons for access showed equivalence of the non pre-stented Hbb-group to pre-stented ureters. Differences in ureteric injury represented small effect sizes, without clinically significant additional morbidity. For post-operative stent duration, Welch's t-test demonstrated moderate to large effect sizes (Cohen's d 0.5-0.8) when comparing Hbb to pre-stented group, indicating a meaningful reduction in stent duration. This suggests that Hbb relaxes ureteral smooth muscle sufficiently to facilitate advancement of ureteral access sheath and flexible ureterorenoscope into the kidney without increasing morbidity.
Comparison with alpha-blockers
Alpha- blockers like tamsulosin enhance UAS placement rates (Nam et al: 88% vs 75%; Dhital et al: 81% vs 60%).8,9 Notably, Dhital et al.9 demonstrated that tamsulosin reduces ureteric injury compared with untreated controls (40% vs 60%), yet injury rates remained substantially higher than in pre- stented patients (40% vs 20%). Nam et al.8 reported elevated injury in tamsulosin arm versus controls (30% vs 15%), a clinically meaningful difference despite lacking statistical significance (p>0.05). By contrast, intravenous HBb achieved renal access comparable to pre- stenting (3.9% vs 1.9% failure) while yielding ureteric injury rates (10.5%) approximating the pre-stented cohort (5.3%), without statistically significant disparity (p>0.05), thereby demonstrating a superior therapeutic profile.
Gastroenterology evidence
In colonoscopy, Hbb is widely used in gastrointestinal endoscopy to facilitate scope passage and mucosal visualization,12 with 85.6% of UK gastroenterologists reporting routine use.10 Its smooth muscle-relaxing effect provides biological plausibility for the observed benefit in urology.
Comparison with other studies
Traxer et al. found ureteral wall injuries with use of UAS in 46.5% of non-pre-stented cases, with severe injuries in 13.3%.5 Taguchi et al.,14 reported ureteral access sheath-related injury in 19.3%, including 9.2% grade 3 injuries. In comparison, overall ureteric injury in the HBb group was 10.5%, substantially lower than published ureteral access sheath-related injury rates.
Strengths
This is a large series (n= 360) from a prospectively maintained audit ensuring data quality and completeness. Both Group A (Hbb) and B (pre-stented) were operated by the author using identical standardized technique/equipment, eliminating operator bias. Group allocation was non-selective: non-pre-stented patients assigned via routine hospital outpatient booking system; pre-stented via emergency ureteric colic admissions – independent of Hbb use. In other words, it is a quasi-randomized study.
Limitations
This study lacks true randomization, even though group allocation occurred via routine clinical pathways. Group B reflects real- world emergency pre-stenting (≥6 weeks), non elective. Small observed differences yield modest post-hoc power, but support Hbb’s benchmarking to pre-stenting. RCT would confirm findings.
Future directions
A randomized controlled trial is warranted to compare Hbb directly with tamsulosin, Hbb combined with tamsulosin, pre-stenting, and placebo.
Intravenous Hyoscine butylbromide at induction in non-pre-stented patients achieves renal access rates comparable to pre- stented RIRS patients, with shorter stent duration, reducing NHS costs from additional procedures and improving QoL by minimizing stent symptoms-a safe single session alternative.
Department of anesthesia, especially Dr Diwakar Subramani and my theatre team
The author declares no conflicts of interest
None

©2026 Gaur. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.