Journal of
eISSN: 2373-6410


Technical Notes Volume 12 Issue 4
11Hungarian Deffence Forces Medical Center 44. Robert K. krt. Budapest 1134 Hungary
2St.Borromeo Hosp.Onitsha, Nigeria
3Department of Maxillofacial Surgery, Semmelweis University, Hungar
Correspondence: Csókay András, Hungarian Deffence Forces Medical Center 44.Robert K. krt., 9.str.Petőfi.Budapest Hungary H-1039
Received: June 12, 2022 | Published: July 27, 2022
Citation: András C, Szeifert GT, Csókay G. How can we reduce the complications in neurosurgical mission? (Daily Fast Fresh Cadaver Practice Help Us). J Neurol Stroke. 2022;12(4):99-100 DOI: 10.15406/jnsk.2022.12.00509
Background: The aim of this article is not to highlight the importance of the advantages of cadaver practice which is fundamental, but to emphasize 3 crucial points. The practice should be: Daily, fast (60-80 min), on fresh cadaver (died within 48 hours, continous venous bleeding present, life like plasticity). Because of development of medical diagnostic procedures in the past half century, unfortunately autopsy dissapeared, it has become unnecessary. Fresh (died within 48 hours) cadaver dissection relatively rare indaily parctice. Our original aim was to reduce the complication rate in very difficult neurosurgical cases. During our work we recognized the extreme advantages of fast daily fresh cadaver pratice; we participated on neurosurgical mission, because of poor medical circumstances where we ought to operate on the same level like in developed world.
Method: In the past 5 years we have introduced; daily fast fresh cadaver dissections for practicing.
Results: Considering the whole time interval operative complications for practicing intern and specialist neurosurgeons have radically decreased as we could sucessfully perform difficult microsurgery in neurosurgical mission as well.
Conclusion: Implementing daily fresh cadaver sessions in a profession where the helpfullness of assisting surgeons is limited would be crucial. Practice on patients is being done currently, is not optimal. “Learning curve” is a “politically correct” expression, but at what cost? A lot of complications behind it. During neurosurgical missions it is impossible to solve neurosurgical difficulties without the highest level of surgical skills.
Keywords: fresh cadaver dissection, neurosurgical mission, practical education
“Hic locus est ubi mors gaudet, succurere vitae” “This is the place where death comes joyfully to aid life” (Gerlei F. pathologist)
Because of solidarity a lot of neurosurgeons organize or participate in neurosurgical missions in underdeveloped countries. The situations alway are unimaginably difficult (Figure 1). None of them are mid-qualified microsurgeon with relatively low number of difficult case experience. They are in the course of learning curve where the complications not rare. During missions we often faced with difficult cases (Figure 1), lacking the equipment used regulary in developed country in Europe or US, Canada etc. How can we improve our skills radically?
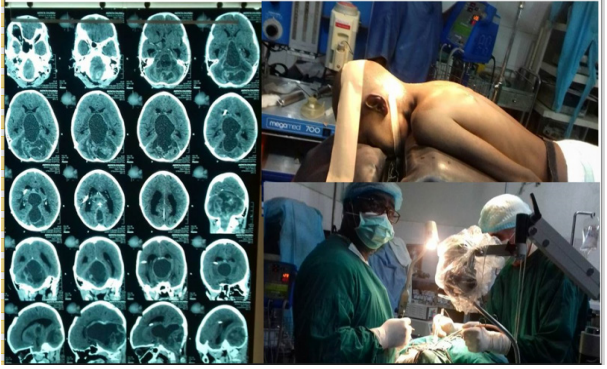
Figure 1 Illustrative case.
Successful removal of cerebellar tumor.(GOS 5) No financical background for post op. ct, only if the patient has life threatening complications. The operative microscope is very simple as the lighting conditions as well.
High level of microsurgery or endoscopic surgery requires virtuosity, which could not be learnt perfectly by assisting because it is mostly an operation requiring one doctor, where the pupils are observing the masters. Practicing on fresh cadavers dates back to hundreds of years. Hundreds of professional articles demonstrate the importance of cadaver practice,1–14 cadaver courses are available all over the world, clinics always are equipped practical anatomic labs, where weekly, monthly practice can be organized. From our experience , in the thousands of regional centers, where the anatomical education is not accessible nor pathology neither forensic study are available.
Considering that, in the developed world, autopsy practically disappeared, the number of cadaver dissections reduced, these type of daily training cannot be performed. As daily practice is indispensable for example in sport.
To order a standard autopsy for educational purposes, it is possible in a lot of developed countries, without the consent of relatives, like in case of organ donations in case of brain death.
There is a possibility, which could bring a great development to microsurgical sciences, instead of practicing on living patients, which is covered by ’politically correct ’ expression ’learning curve’. In reality, behind this statements there are a lot of human tragedies, severe complications.
We have to highlight that complications are not the results of malpractice, but possible complications are acknowledged by the patients and doctors prior treatment. Obviously, daily training is necessary as it is for sport champions or virtuoso pianists, violinists. It seems to be straightforward, but why has not it become part of daily practice rutine? Why are not we capable of performing autopsy on a daly basis. Performers do not practice at competitions or performances, they do not test their new creative ideas on the spot when competing.
We gained meaningfull results in the field of practical education and sciences. Most importantly, the quality of daily neurosurgical care increased dramatically. Benefits were experienced in neurosurgical missions in Africa (3 times 2 weeks long mission) where the circumstances were very poor. Under poor working condition our practice should be automatic even if the pathology is challenging. Our mental and physical capacity is needed for defeating the poor conditions many creative options should be used during the operations.
We have been doing this project for 15 years, (first author) firstly 2-3 times / week and 5 years ago I switched to practicing on a daily basis. We modellize the most demanding intraoperative situations every day, creating arteficial complications on vessels and reparing by microvascular sutures, in the deep on the skull base.
Daily fresh cadaver practice during the neurosurgical missions also beneficial where the professional circumstances are very limited. Neurosurgeons from developed country need to help for underdeveloped world. We need a change in practical education by every day practicing. We apply the contemplative Jesus prayers in the course of fresh cadaver practicing and living operations as the one of the sources of neurosurgical innovations in mission.15 It is personal experince of first author (Figure 2).
None.
The authors declare no conflicts of interest.

©2022 András, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.