Journal of
eISSN: 2373-6410


Literature Review Volume 12 Issue 5
1Faculdade de Medicina, Centro Universitário Christus, UNICHRISTUS, Brasil
2Universidade Federal de São Paulo, Brasil
3Laboratório de Neurociências, Departamento de Neurologia e Neurocirurgia, Universidade Federal de São Paulo, Brasil
4Laboratório de Neuropsicofarmacologia, Núcleo de Pesquisa e Desenvolvimento de Medicamentos, Universidade Federal do Ceará, Brasil
5Centro Universitário Barão de Mauá, Brasil
Correspondence: Júlio César Claudino dos Santos, Departamento de Neurologia e Neurocirurgia, Universidade Federal de São Paulo, Rua Sena Madureira, 1500,Vila Clementino (SP), Brasil, CEP 04021-001, Tel 55-19-984506660
Received: August 25, 2022 | Published: September 6, 2022
Citation: Sallem CC, Filho LBA, da Costa RI, et al. The role of gut-brain axis in mood disorder. J Neurol Stroke. 2022;12(5):138-146. DOI: 10.15406/jnsk.2022.12.00516
The connection between the gastrointestinal system (GI) and the central nervous system (CNS), together with the performance of the enteric nervous system (ENS), forms a complex communication network called the “gut-brain axis”. Scientific evidence indicates that the gut microbiota coordinates a multitude of bodily functions, closely linked to the immune, metabolic and nervous systems. In this context, any alteration that occurs in the “gut-brain axis” will result in damage to the homeostasis of the systems, because a dysfunction of the intestine-brain axis can lead to a dynamic impairment of the action of the protective barriers of the intestinal walls. Through directional gut-brain communication, the changes detected in the gastrointestinal tract affect the neurochemical transformations that occur in the CNS. The recognition of the relationship of neural aspects to the dynamics of the human microbiome contributes to the emergence of physiological imbalances that can contribute to the worsening of a wide spectrum of psychiatric disorders, with emphasis in the literature on anxiety disorders, depression, and autism spectrum disorders (ASD), schizophrenia and attention-deficit hyperactivity disorder (ADHD). The present literature review aims to verify the function and impact of the gut-brain axis in mood disorders, aiming to identify and strengthen evidence that the brain and gut have a strong and intimate connection responsible for the modulation of neurons, neurotransmitters, hormones and immunological mediators.
Keywords: gut-brain axis, mood disorders, microbiota, neuropsychiatric disorders, neurological diseases
Mood disorders are part of a group of diseases associated with physiological, psychological, genetic, physical, chemical and cultural dysfunctions. Besides, these disorders present cognitive and behavioral alterations which damage the personal, social, professional and familial relationships.1 Globally, the Pan-American Health Organization (PAHO) points out that mood and mental disorders represent 12% of the world´s diseases and 1% of mortality, while the investment in resources for mental health actions is less than 1%.2 Nationally, the World Health Organization (WHO), through the International Consortium in Psychiatric Epidemiology (ICPE), observed that, amongst Latin America countries, Brazil has the greatest prevalence of mental disorders in the adult population (15-59 years).3,4 Thus, the Ministry of Health reports that 3% of the Brazilian population suffers from some severe and persistent mental disorder,5 amongst them: psychosis, mania, schizofrenia, anxiety, depression, bipolar and compulsive-obsessive disorders.6
Having this information, the Global project “Burden of Disease”, from 2017, highlights the impact of mental disorders in society, since these dysfunctions represent the second global cause of incapacity.7 Accordingly, it is valid to comprehend that the pathophysiology of these diseases is linked to the monoaminergic system, originated in small nuclei in the brain stem (locus coeruleus, raphe nuclei and substantia nigra) mainly in the mesencephalon, and that projects itself through the cortex. This system is integrated by neurotransmitters, such as norepinefrin (NE), serotonin (5-HT) and dopamine (DA), that act in the modulation and integration of cortical and subcortical activities and play determining parts in the individual's behavior, besides, it is also responsible for some motor and cognitive functions.8 Furthermore, the prefrontal cortex keeps intimate connections with the paralimbic pathways, linked to emotional aspects, since this area is activated in the generation of sad thoughts.9 Nonetheless, other physiological pathways that impact directly in mood disorders can be analyzed, for example the gastrointestinal system.
Accordingly, the human intestinal tract accomodated over 100 trillion bacteria. One of the functions performed by these microorganisms is the secretion of neurotransmitters - for example the gamma-aminobutyric acid (GABA), serotonin (5-HT) and glycine - which act in the treatment of mood disorders. The reason for this is that the neuroactive molecules present in the intestinal microbiota have the capacity to regulate nervous signals and can affect neuropsychiatric patterns, such as: sleep, appetite, mood and cognition.10 Effectively, studies report that the composition of the intestinal microbiota and its microbiome can be potent modulators of cerebral processes, such as mielinizacion, neurogenesis and microglia activation, and also be an agent in the prevention of neurodegenerative and neurodevelopmental disorders.11 According to this, it is observed that some neurotransmitter alterations in a situation of mental dysfunction cannot be originated in the disorder itself, but in an irregularity of the intestinal microbiota.12
Thus, the existing relation between the gastrointestinal (GI) system and the central nervous system (CNS) is denominated “gut-brain axis” and consists of the bidirectional exchange between these two systems. Besides, the formed communication network is of complex nature and also includes the enteric nervous system (ENS), known as “second brain” for containing millions of ganglia and about 400 million neurons, approximately the same quantity of neurons of the spinal cord, this system is formed by the digestive tract and also extends itself between the esophagus and the anus.13 The ENS, associated to branches of the sympathetic and parasympathetic autonomic nervous system (ANS), is involved with functions linked to the control of the gastrointestinal motility, sensations, regulation of fluid exchanges, local blood flow, gastric and pancreatic secretion, gastrointestinal endocrine functions, defense reactions and enteroenteric reflexes. The main gut-brain connection pathways occur through the vagus nerve, tryptophan metabolites and microbial products, such as short-chain fatty acids. Together, those will stimulate brain function, modulating the serotoninergic, noradrenergic and dopaminergic neurotransmission.14,15 Thus, the emerging evidence indicates that the intestinal microbiota coordinates a multiplicity of body functions, intimately linked to the immune, metabolic and nervous systems. In this context, any alteration that occurs in this axis will repercute in damages to the systems homeostasis.16
Furthermore, the indications that the microbiome orientates the gut-brain axis caused a change of paradigm in which concerns the pathophysiology of mood disorders, since the psychological stress and systemic inflammation are common denominators in the disorders in which the microbiota can execute therapeutic effects. Thus, the stress would be linked to disorders such as depression, schizophrenia and autism spectrum disorder (ASD), whilst the inflammation is also linked to depression, schizophrenia and Parkinson's disease.13 In this perspective, the gut-brain axis comprehends a biochemical signalization pathway between the gastrointestinal (GI) structure and the central nervous system (CNS), since when that presents any dysfunction, the action of the intestine´s walls protecting barrier is compromised, enhancing intestinal permeability and, consequently, the penetration of substances that affect other physiologic functions.15 These events can be the origin of diseases, amongst them a broad spectrum of psychiatric disorders, once they lead to the activation of the innate immune response, which will cause a chronification of the high levels of inflammatory mediators.17,18
Regarding the development of research about the gut-brain axis, many were performed in animal models, for example germ-free, genetically modified and antibiotic treated mice. These animals have been essential tools for the comprehension of the relations between microorganisms and its host, since the results provide information about how the microbiota is fundamental in the formation of behavior, physiology and neurobiology of its host. In those studies, it was observed that animals with no microbiota have a complete distinct development when compared to animals that host commensal bacteria in their microbiotas.13,19 In contrast, a lower number of clinical studies investigated if the interactions observed in rodents are also observed in humans. Thus, there is still scarce evidence about the mechanisms that associate the microbiota to the communication of the gut-brain axis.20,21
According to the information exposed, taking into consideration the reported number of cases about diseases linked to mood disorders and the negative repercussion in public health caused by these diseases, the present study bases its investigation in the functioning of the gut-brain axis, aiming to identify and strengthen the evidences that the brain and the intestine have a strong and intimate connection responsible for the modulation of neurons, neurotransmitters, hormones and immune mediators. Beside, this trial will allow the understanding of another possible way of treatment and the prevention of neuropsychiatric and neurodegenerative diseases though a new therapeutic approach.
The present study consists of a literature review performed in the PubMed, Science Direct e Scielo databases, published between 2017 and 2022, which had the objective of verifying the function and the impact of the gut-brain axis in the mood disorders. The search for articles utilized as a direction the following keywords: gut-brain axis; mood disorders; microbiota; neuropsychiatric disorders; neurologic diseases. Thus, in the PubMed database, 257 articles were identified by the utilized Mesh descriptor “(GBA) AND (MD)”, 36 amongst those were selected, after Selection I. Still referring to the PubMed platform, the “(GBA) AND (NPO) AND (pathophysiology)” description was utilized, finding 61 articles, from which 22 were maintained for the next stage. The first exclusion criteria consisted in the elimination by titles that did not contain the topic “gut-brain axis correlated to neurologic disorders”, as well as not comprehended in the predefined period.
Subsequently, through the Science Direct database, when utilizing the description “(GBA) AND (MICROBIOTA) AND (ND)” 134 articles were identified between 2021 and 2022, from which 13 were selected. The exclusion criteria for this database was the absence of connectivity between the microbiota dysfunctions and neurologic diseases. Furthermore, the last platform visited was Scielo, with the research directed by “(MTD) AND (epidemiology)”, in which 79 articles were discovered, from which 15 were selected, by observing the title related to the epidemiology of the psychiatric diseases, finishing the identification phase and Selection I.
When entering Selection II and Eligibility, the second exclusion criteria was applied, having as analysis the articles´ abstracts and the elimination of those that did not present information that addressed or ratified the gut-brain axis´s function in the context of mood disorders. As a result, 42 articles were excluded and 44 were maintained for the Eligibility stage. Subsequently, 56 more articles were validated, since they brought additional information about animal tests that reinforce the research. Finally, in the Inclusion stage, a total of 100 original articles in English and Portuguese (including books, guidelines, chapters and case reports) remained.
Through the selection of articles, it was possible to produce a table that presents some mood disorders associated with the gut-brain axis. In addition, the identification of relevant information on the topic under study serves to support the importance of the work in progress. Thus, the table consists of data referring to the authorship of the article, the title of the productions, the diseases correlated to the current topic and the conclusions of each research. Therefore, the analysis of the results found was more efficient, making it possible to clearly visualize the considerations that will be exposed in the discussion (Table 1).
|
Author, year |
Title |
Objective |
Correlated disorders |
Results/ |
|
Socala et al.22 |
The role of |
Present recent data on the role of the microbiota-intestine-brain axis in the pathophysiology of neuropsychiatric and |
Depression, anxiety disorder, schizophrenia, autistic spectrum |
The gut microbiota is increasingly recognized as an important player in the pathophysiology and treatment of neuropsychiatric disorders. However, the cause-effect relationship is still inconclusive. |
|
Generoso et al.17 2021 |
The role of the |
Review the interaction and alteration that the microbiota performs in the brain and vice versa, and to expose the impacts of this relationship on human behavior and the |
Anxiety disorder, autistic |
The evidence presented in this article indicates a close relationship between the microbiota and mental disorders. However, a deeper study of tryptophan metabolites and their functional implications at different stages of life is needed. This will eventually help clarify how the |
|
Chang et al. 23 2022 |
Brain-gut-microbiota |
Present and discuss the brain- |
Depression |
The gut-brain axis is considered a new paradigm with the potential to provide therapeutic strategies for |
|
Foster et al.24 2021 |
The relationship |
Investigate the relationship and interactions of the microbiome with major depressive disorder |
Major depressive disorder (MDD) |
There are relevant indications to consider the microbiome as an alternative for clinical psychiatric |
|
Patrono et al.25 2022 |
Schizophrenia, |
Review the recent findings on the relationship between gut microbiota and schizophrenia. In addition, evaluating the manipulation of actors in the brain or gut may improve potential treatment research. |
Schizophrenia |
The investigations on the |
|
Gambaro et al.26 2020 |
Review of the role of the probiotics in anxiety and effectiveness of probiotic depressive disorders. |
Identify data, investigate the effectiveness of probiotic consumption on improving depressive symptoms, anxiety symptoms, quality of life and inflammatory biomarkers. |
Anxiety disorder, depression |
The results for depression treatment with the gut-brain axis as a starting point are encouraging, but more research is needed, considering the scarcity of clinical trials on this topic and the heterogeneity of the analyzed samples. |
|
Li et al.27 2017 |
The Gut Microbiota and Autism spectrum Disorders |
Analyze the bidirectional between the central nervous system and brain-intestine axis and the role of the gut |
Autistic spectrum disorder (ASD) |
The literature has shown that an abnormal gut microbiota is related to SAD. In addition, many |
|
Kunugi et al.28 2020 |
Gut Microbiota Pathophysiology of Depressive Disorder |
Connect the evidence of the pathophysiology of the |
Major depressive |
|
|
Mathee et al.29 2020 |
The gut microbiome and neuropsychiatric disorders: implications |
Demonstrate the importance and extreme need for a comprehensive and in-depth analysis of the role of the gut |
Attention deficit/Hyperactive disorder |
Understanding the impacts of the gut microbiome on relevant neuromodulators and compositional |
|
Longsha et al.30 2019 |
Microbiota and the gut brain axis: Implications for new therapeutic design in the CNS |
Uncover the complex interactions of the microbiota-gut-brain-axis: intestine-brain axis to establish Implications for new therapeutic design in the a better understanding of microbiota-mediated CNS pathogenesis, pathways to non- |
Autism spectrum disorder (ASD), depression, anxiety, stress and schizophrenia. |
The evolution of the microbiome field has allowed a significant step closer to understanding CNS disease treatments by unraveling the complex networks of the immune system, gut microbiota, and microbiota-intestine-brain axis. The study concluded that |
Table 1 Summary of results
The recognition of the neural aspects associated with the dynamics of the human microbiome contributes to advances in the treatment of pathologies of a psychic nature that can be treated by alternative, but equally efficient means, highlighting the object of this work: the gut-brain axis (GB). Based on the results achieved, it is worth discussing the main disorders investigated in the literature: anxiety disorder, depression, autism spectrum disorder (ASD), schizophrenia and attention deficit hyperactivity disorder (ADHD).
Anxiety disorder
The development of mood disorders, especially anxiety disorder, depends on genetic and environmental factors. In addition to these, another relevant aspect that may be related to this disease is the composition of the microbiota,31 which communicates with the brain through some pathways, such as the vagus nerve, tryptophan metabolism, the immune system and the enteric nervous system (ENS), which ends up involving peptidoglycans, branched-chain amino acids, microbial metabolites and short-chain fatty acids (SCFAs), which may have changes influenced early in life by infections, antibiotics, type of delivery, stress, genetics, and nutrition.19 Thus, preclinical behavioral and biochemical studies have found that the presence or absence of conventional gut microbiota influences the development of anxious behaviors and is accompanied by neurochemical changes in the central nervous system (CNS).13
In this context, the evidence brought by these studies link anxiety to the gut-brain axis. In a comparison between a group of patients that received the administration of probiotics and another group that used a placebo, it was revealed that the plasma levels of cortisol, as well as plasma pro-inflammatory cytokines, were lower in subjects that received probiotics than placebo, resulting in the improvement of the symptoms of the disease.17
In parallel with the experiments carried out in humans, tests carried out in mice and other rodents showed that the presence and composition of the intestinal microbiota can alter the emotional reaction of animals. In mice, for example, infections and intestinal inflammation caused an increase in behavior patterns thought to represent anxiety, including decreased exploration and increased behavioral inhibition.19,32 Indeed, the presence of potentially pathogenic and intestinal inflammatory bacteria stimulates immune pathways in the body, acting on the activation of microglia (immune cells residing in the CNS) and on the production of short-chain fatty acids (SCFAs), as a way to restore the health of the intestinal microbiota.33
In addition to the immune system response, prebiotics and probiotics, studies bring another powerful biological mechanism as an anxiolytic effect: the production of neurotransmitters, such as serotonin.13 Serotonin (5-hydroxytryptamine) is an important neuronal and endocrine signaling agent, acting in the regulation of appetite, sleep patterns, mood and cognition.33 Although this substance is synthesized by ENS neurons, more than 80% of serotonin is produced in the gastrointestinal tract by species of Lactococcus, Lactobacillus, Streptococcus, among others.34,35 In this sense, enteric serotonin levels are regulated by tryptophan TPH1 and its expression is induced by high levels of SCFAs, associated with a decrease in anxiety and depression-like behaviors.30,36,37
Finally, it is worth mentioning that the bidirectional communication of the gut-brain axis also has other neurotransmitters, such as dopamine, gamma aminobutyric acid (GABA), acetylcholine and norepinephrine, which are active in the regulation of mood disorders, especially anxiety and depression,33,38 which is the next topic of discussion in this review.
Depression
According to the Global Health Data Exchange (2021), 280 million people of all ages are affected by depression worldwide, in addition to being the most common mental disorder and one of the most disabling. Despite the amount of research on the disease, the mechanisms underlying the pathophysiology of depression are still unclear. However, the results obtained in clinical studies suggest that alterations such as, for example, the intestinal microbiota, the amount of short-chain fatty acids, amino acids, and microbial-derived metabolites play a relevant role in the pathophysiology of depression via the gut-brain (GB) axis.21,23
From this perspective, the accumulated evidence suggests that the brain-gut-microbiota (BGM) axis is responsible for the pathophysiology of depression. Changes in the gut microbiota have been increasingly characterized in patients with depression.24,26 One example is the large-scale metagenomic study with 1,054 volunteers that confirmed the existence of a close relationship between gut microbes, dietary health and depression. That's because butyric acid-producing Faecalibacterium and Coprococcus bacteria have been identified as important indicators of a high-quality diet, even in patients with depression treated with antidepressants.39
Thus, the GB axis is considered a new paradigm with the potential to provide new treatment strategies for depression, given that it is a complex and interactive system that includes a network of neural, immunological and chemical signals. All these networks appear to be involved in the pathophysiology of depression.23,40,41
Therefore, targeting the GB axis of the beneficial effects of diets and psychobiotics (a class of probiotics that support the microbiome of people suffering from psychiatric disorders) has been increasingly reported in preclinical and clinical studies.23,28 Despite this, a greater understanding of the dynamics of this axis (GB) in depression is necessary before applying this system as a therapeutic alternative for mental health.26,33
Autism
Autism spectrum disorder (ASD) or autism is a condition characterized by restricted or repetitive behavior of the individual, as well as difficulties in communication and social interactions. Therefore, although it has a genetic origin, environmental factors can lead to the potentiation of symptoms and aggravations of the disorder.34
In this context, research has shown that 90% of individuals diagnosed with autism suffer from dysbiosis. This data led researchers to observe that autistic patients present a significant increase in Clostridium, Clostridium hathewayi and Clostridium orbiscindens defense cells; in smaller amounts, the presence of Faecalibacterium and Ruminococcus spp was detected.38 The clinical relevance of the finding is that these latter species of bacteria have anti-inflammatory properties, while most Clostridium spp are considered commensals with a fundamental role in the maintenance of intestinal homeostasis.27,40
In view of this, patients with ASD have the homeostatic state of the microbiome altered by diets with pro-inflammatory foods, medication regimens, medical comorbidities, and acute and chronic gastrointestinal symptoms. Based on this, since the gut-brain axis is a bidirectional communication pathway, the importance of the system in the pathogenesis of ASD grows.36,42,43
Despite advances regarding the therapeutic potential of ASD associated with the gut-brain axis, a significant effort is also needed in the investigation of the brain-gut axis in adults with ASD, as almost all research in this area has focused on the pediatric population.40 Despite this, understanding the mechanisms that cause dysfunction in brain-gut communication may lead to a greater understanding of the underlying pathophysiology of the brain-gut axis in patients with ASD. Furthermore, it may reveal new therapeutic targets, given the growing evidence suggesting that one of the main modulators of gut-brain communication in ASD is the gut microbiome.41,42
Schizophrenia
Schizophrenia is a psychiatric and neurodegenerative disorder considered as one of the top 15 leading causes of disability worldwide in 2016,44 affecting 0.3 to 0.7% of the global population.45 The prevalence in men and women is similar,46 but the clinical manifestations tend to start sooner in men and with increased severity, with the first symptoms starting at the end of adolescence and the beginning of adulthosod.47 The reduction in life expectancy is between 10 and 20 years,48 being 10% of mortality rate associated with suicide.49 The main cause of mortality is due to cardiovascular diseases, being correlated with the increased exposition of cardiovascular risk factors such obesity, tobacco, diabetes, and unhealthy lifestyle.50 Interestingly Coprococcus sp was associated with higher risk for coronary heart disease in schizophrenia patients.51–55
The symptomatology is composed by positive symptoms (delirium, hallucinations), negative symptoms (avolition, anhedonia, social withdrawal, poverty of speech), cognitive deficits (attention, working memory and executive function) and humor/anxiety symptoms, in a complex interaction that results in thousands of variants.56 The etiology involves the interaction of genetic vulnerability with environmental factors. Significant increased risk (10-20 times) for developing schizophrenia and schizophrenia spectrum disorders was associated after prenatal microbial infection,57 such as Toxoplasma gondii and Influenza and increase cytokines, such as IL-8, TNF-alpha and C reactive protein.22,58 Interestingly, prenatal administration of poly I: C (synthetic analog of double-stranded RNA used to stimulate viral infections), which proves that prenatal immune activation by infection can negatively affect all the development of mesocorticolimbic dopaminergic system.59,60
Schizophrenia patients have elevated incidence of intestinal barrier dysfunction (‘’leaky gut’’),61 increase bacterial translocation and gastrointestinal (GI) comorbidities associated with inflammation,62 these results highlights the involvement of the microbiota-gut-brain axis in the disease. Interestingly, it was demonstrated that fecal matter transplant from patients with schizophrenia to germ-free (GF) mice may produce schizophrenia-related changes in animal behavior, with increased levels of glutamate and decreased levels of glutamine and GABA in the hippocampus.63 Also, the findings of bacterial translocation and GI inflammation correlates with the central pathology of schizophrenia, as the increase of inflammatory cytokines (IL-6) activates the enzyme indoleamine-2,3-dioxygenase, intensifying tryptophan to the kynurenine metabolism resulting in the increase of the production of kynurenic acid, a natural antagonist of N-metil-D-aspartate (NMDA) receptor, which is involved in schizophrenia pathology.64 Furthermore, altered tryptophan-kynurenine metabolism may be an important link between gut microbiota and the pathogenesis of schizophrenia.65
Exclusive administration of Streptococcus vestibularis in mice with antibiotic-depleted microbiota resulted in hyperkinetic behavior, impaired social interaction, transcriptional changes in genes involving inflammation factors and altered neurotransmitters in peripheral tissues. Vestibular Streptococcus, known to enter the brain, is present in several schizophrenic patients being identified as having 11 gut-brain modules that synthesize and degrade neurotransmitters such as glutamate and GABA.65,66
It is difficult to determine the mechanism by which intestinal microbiota contribute to the development of schizophrenia, because of the limitations and the current lack of an animal model of schizophrenia covering all the complexities of the disease.62 However, in animal studies, postnatal development and maturation of the neural, immune, and endocrine system, often disturbed in schizophrenia patients, was intrinsically associated with gut microbiota.67 Also, in GF animals, it was demonstrated an altered stress responsivity, with excessive activation of the hypothalamic-pituitary-adrenal (HPA) axis in response to stress exposure and decreased glucocorticoid receptor expression in the hippocampus, correlating with schizophrenia neurochemical and molecular alterations.58
Also, unique bacterial taxa, such as Veillonellaceae and Lachnospiraceae, were associated with severity of schizophrenia.68 In a recent study, Shen et al. (2018) compared 64 patients with schizophrenia and 53 healthy controls, finding in schizophrenics higher numbers of Proteobacteria, Succinivibrio, Megasphaera, Collinsella, Clostridium, Klebsiella and Methanbrevibacter and a lower number of Blautia, Coprococcus, Roseburia compared to healthy controls.69 However, He et al.70 demonstrated no significant difference in microbial diversity between high-risk patients, ultra-risk patients and healthy controls. Also, most studies correlating microbiota differences between schizophrenia patients and control groups used unadjusted P values or not even inform its values, raising false-positive discoveries, that may be due to confounding factors such diet, age, treatment status, differences in the stage of illness or small sample sizes (< 100 individuals).58 Although increased abundance of Lactobacilli seems to be the most consistent finding so far, the available data is inconclusive on dysbiosis increasing the potential of someone to develop schizophrenia.
Attention deficit hyperactivity disorder (ADHD)
Attention deficit/hyperactivity disorder (ADHD) it’s a developmental neuropsychiatric disorder associated with abnormalities in dopamine, serotonin and noradrenaline neurotransmission, including inattention, hyperactivity and impulsivity that interfere with daily functioning and development.71 It normally starts in childhood and can persist into adulthood. The world-wide prevalence of ADHD is around 5% in children72 and 2,5% in adults.73 In children, it's more prevalent excessive, persistent and age-inappropriate symptoms of inattention, hyperactivity, and/ or impulsivity. In adolescence, inattentive symptoms are more prevalent, with declined hyperactive and impulsive symptoms. In adulthood, inattention persists or even increases.74 Although ADHD has been described as being 2 to 3 times more prevalent in boys than in girls, this may be due to the fact that girls have less excessive motor symptoms and boys have more oppositional defiant disorder (ODD), which contribute to the increase in boys diagnosis.75
In relation to genetics, ADHD is one of the most heritable psychiatric disorders, with 70 to 80% of variability attributed to genetics factors.76 In that way, the clinical diagnosis of ADHD it’s been considered an extreme of a biological trait.77 In the other way, environmental influences include prenatal factors (maternal stress, smoking and alcohol use during pregnancy), perinatal factors (stress, premature birth, low birth weight, breastfeeding), maltreatment and environmental toxins exposure.78
The study of the gut microbiome of ADHD is still at the beginning and encounter some difficulties,79 as it contains overlapping symptoms with autism-spectrum disorder (such, limited areas of focus, social awkwardness and impulsivity) or even the two disorders co-exists in 28% of ADHD diagnostics, according to a recent meta-analysis.80 However, it has been described in ADHD children a higher incidence of gastrointestinal symptoms, such as constipation.81–83
A significant association between ADHD and obesity has been made,84 and it has been proposed that ADHD symptoms, such as impulsivity and emotional distress, may predispose to poor dietary choices (ie, fat-rich or sugar-rich foods) to compensate for the emotional burden as a form of self-medication.85 Also, ‘’Western’’ type diets were significantly associated with ADHD diagnosis86 and it has been described that patients with ADHD tended to eat at fast-food restaurants and skipped breakfast more often than controls.87 Interestingly, skipping breakfast or substituting for a sugary drink impairs attention and episodic memory in children.88 Also, iron and zinc deficiency (low plasma levels), cofactor of dopamine and norepinephrine, were found in children with ADHD,89 which demonstrates the role of diet in the etiology and worsening of ADHD. Interestingly, a vicious cycle that includes impulsivity and family dysfunctions leading to worse food choices and then to a low intake of nutrients has been made.87 Additionally, Omega-3 supplementation was found to reduce symptoms of ADHD90 and to reduce oppositional defiant disorder in children with ADHD.91
In relation to the microbiota in ADHD patients, an increase in the genus Bifidobacterium was found, appearing to be solely responsible for the increase in cyclohexadienyl dehydratase (CDT) enzyme, responsible for the synthesis of phenylalanine (which cross the blood-brain barrier), a precursor of dopamine. High levels of phenylalanine have been linked to ADHD symptoms,92 and these ADHD patients with an increase of Bifidobacterium demonstrated a reduced brain reward response, modulated by dopamine in striatal BOLD response for reward anticipation.93 Also, gut microbiota was associated with mRNA expression of D1 (dopamine) receptor, higher in the hippocampus in GF mice and with a higher turnover rate in the striatum.94 This association constitutes the metabolic pathway that up to date, rather than the vagus nerve pathway and the immune pathway, has the most causality correlating gut microbiota to executive functions in ADHD,83,95 although other ADHD specific metagenomic profiling of patients compared to control has also been described.96
ADHD was also associated with a higher incidence of auto-immune diseases, such as ulcerative colitis, diabetes mellitus, atopic dermatitis, allergic rhinitis, ankylosing spondylitis97,98 which has been associated with dysregulation of inflammatory mechanisms and microbiota alterations.99 Interestingly, adverse behavior, as seen in ADHD, can also be caused by food sensitivity, which is like an allergic reaction in atopic diseases.99 Also, atopic symptoms severity correlates to ADHD prevalence, which indicates a shared genetic association between atopic diseases and ADHD,100 as can be seen in Figure 1 & 2.
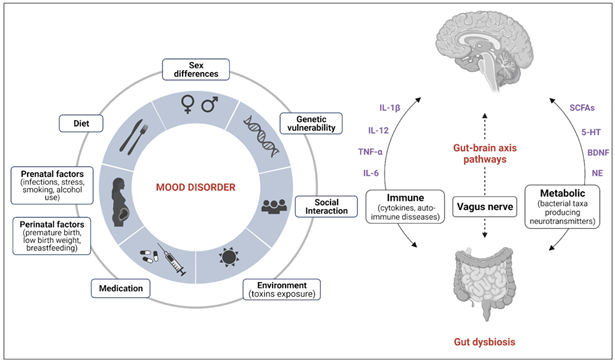
Figure 2 Bidirectional pathways of the gut-brain axis in mood disorders.
The development of mood disorders can be associated with a plethora of interactions of the gut, such as diet, sex differences, genetic vulnerability, enviroment, social interactions, medication and pregnancy outcomes (eg. prenatal factors and perinatal factors). Also, the gut and the brain's bidirectional communication it's been described to be made through an immune, metabolic and nervous pathways.
Based on the studies reviewed, it can be concluded that changes in the intestinal microbiome, such as the presence or absence of types of bacteria, defense cells (responsible for the immune response and association with the HPA axis) and neurotransmitters synthesized by the ENS are closely linked to the etiology of mental disorders. Through gut-brain directional communication, changes detected in the gastrointestinal tract have repercussions on neurochemical transformations in the CNS. Thus, it is observed that the growth of research on the relationship between the gut-brain axis and mood disorders is still in an exploratory phase, but there is evidence that intestinal modulation promotes a positive effect on the regulation of mood state, helping to support the rationale of potential of this system as a therapeutic alternative for mental illnesses.
Medical School of University Center Christus, UNICHRISTUS, Fortaleza, CE, Brazil.
The authors declare that they have no conflicts of interest. All authors read and approved the final manuscript.

©2022 Sallem, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.