Journal of
eISSN: 2373-6410


Case Report Volume 11 Issue 4
Hue University of Medicine and Pharmacy, Hue University, Vietnam
Correspondence: Dinh Thi Phuong Hoai, Hue University of Medicine and Pharmacy, Hue University
Received: July 13, 2021 | Published: August 6, 2021
Citation: Hoai DTP, Dung NTM, Cuong HM, et al. Warning with chronic subdural hematomas in the elderly. J Neurol Stroke. 2021;11(4):114-117. DOI: 10.15406/jnsk.2021.11.00467
Chronic subdural hematoma (cSDH) is a disorder in which blood collects between the dura and arachnoid mater of meninges around the brain. It's more common among the elderly and usually triggered by a head injury. We report a case of a 78-year-old male patient who had previously been diagnosed with a left hemisphere subdural hematoma for no apparent reason with a history of hypertension. Two days before hospitalizing, he had a symptom of weakness in the right extremities. Non-contrast CT of head reveals a crescent-shaped, heterodense lesion over the lateral aspect of the left hemisphere measuring 11x5x1 cm with mass effect to the adjacent brain parenchyma. Burr hole drainage was performed for the patient. His symptoms improved after the surgery.
Keywords: chronic subdural hematoma, elderly, intracranial hematoma, head injury
Chronic subdural hematoma (cSDH), is a collection of blood accumulating in the subdural space, is a fairly common condition in neurosurgery, with an incidence of about 5/100 000 of the general population and increased to 58/100 000 population for the group over 70 years old.1 Nowadays, the elderly population in developed countries increases, so the rate of cSDH also increases.1
It is mainly caused by head trauma causing rupture of blood vessels and a small percentage by primary bleeding. Risk factors for cSDH are often associated with brain atrophy such as older age, alcoholism, people with dementia (Alzheimer's disease), use of anticoagulants or antiplatelet drugs.2,3 Common symptoms of cSHD are headache, confusion, hemiparesis, personality changes, and occasional seizures.2 These symptoms are often gradual and difficult to detect the disease.
The elderly are at a higher risk of cSDH due to an increased risk of falls, while brain contraction in the elderly further exacerbated by chronic alcohol abuse is also thought to be a contributing factor as it results in tension on the bridging vessels, which then easily tear during minor head blows or trauma.2 People with underlying medical conditions such as hypertension and diabetes are also at risk for cSDH.4 They may confuse symptoms of subdural hematoma with other diseases such as dementia, stroke (cerebrovascular accident), transient ischemic attack, as well as symptoms of confusion, headache, which are very common symptom in the elderly, so cSDH is easily forgotten.
In this case, we report a case of bleeding secondary to chronic subdural hematoma in a 78-year-old patient with a previous diagnosis of SDH more than two months ago. The purpose of this report is to: review the literature, clinical symptoms, and imaging studies to help raise awareness of chronic subdural hematoma in the elderly.
A 78 years old male patient, was admitted to the Department of Neurosurgery, Hue University of Medicine and Pharmacy Hospital with right hemiplegia, which started 3 days before admission. Two and a half months ago, he fell, hit his left head on the ground, had to go to other hospitals for examination and was diagnosed with a left subdural hematomamonitored and treated conservatively. The patient has a history of well-controlled hypertension. On admission, the patient was alert, well-contacted, GCS:15 points, blood pressure 140/90 mmHg, pulse 95 times/minute, respiratory rate 20 times/minute, temperature 37oC, right hemiplegia, Muscle strength of right arm is 3/5 and right leg is 4/5, left arm and leg are 5/5, no facial paralysis, no blurred vision, no dizziness, no tinnitus. Other organs have not detected abnormalities. On a CT scan of the brain without contrast, the image of a crescent-shaped mass in the left frontotemporal region of the brain with mixed density increased and decreased, about 11x5x1cm in size, compressing the adjacent parenchyma (Figure 1A-1C). The diagnosis was made in the patient as secondary bleeding on the background of chronic left hemisphere subdural hematoma. In addition, on a CT scan, brain atrophy can be seen quite clearly. The results of hematological tests were within normal limits. Chest x-ray showed a mild right pleural effusion.
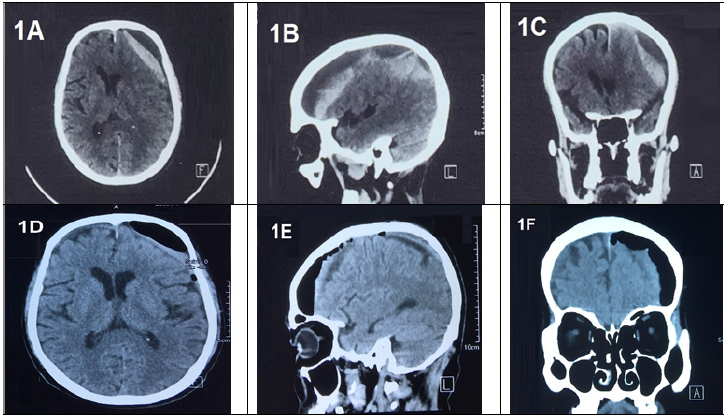
Figure 1 Figure 1A-C CT-scan of the brain without contrast shows a crescent-shaped mass in the left frontotemporal region of the left brain with a mixed density of increase and decrease, in size 11x5x1cm, compressing the adjacent parenchyma.
Figure 1D-F Postoperative CT-scan of the brain shows that the hematoma remains about 80% of the baseline and pneumocephalus.
The patient was operated by the method of Burr hole evacuation. After endotracheal anesthesia for the patient, a 3cm incision was made on the left top of the head skin, drilled a hole in the skull, burned the dura, showed black blood, rinsed, and placed drainage outside the skull. Finally, close the 3-layer incision. One day after surgery, the patient is awake, the vital signs are stable, and a CT scan is indicated (Figure 1D-1F). Currently, the patient's health has been restored, the right hemiplegia has improved (Figure 2).
A subdural hematoma, as its name implies, forms because of an abnormal collection of blood under the dura mater. This is one of the intracranial injuries associated with abusive head trauma. Our patient may initially be asymptomatic, after 3 weeks even a few months after symptoms appear, this easily makes patients forget that they have previous trauma and access to treatment relatively late, cSDH is mostly seen in elderly people, average age 60 years. More men than women, the most common cause is a traumatic brain injury.
The pathogenesis of cSDH is explained as follows: The collision damages the cortical vein where the blood vessels drain into the superior sagittal sinus or the bridging vein causing hemorrhage in the dural space. Over the next two weeks, the hematopoietic process takes place, with the appearance of a membrane surrounding the hematoma to form a fluid cyst. The fluid cyst consists of two membranes: the dura and arachnoid mater of meninges, which can be calcified.5 More than half of the cases of subdural hematomas are liquefied and tend to increase in volume.6 This is explained by three causes, due to recurrent bleeding from the bypass veins or neovascularization of the hematoma periphery, an inflammatory reaction and fibrinolysis occurring leading to hemorrhage, when the hematoma increases the osmotic pressure at the outer membrane of the fluid capsule, so water is absorbed into the hematoma.5 As a final consequence, the hypervolemic mass causes a space-occupying effect and the patient begins to develop symptoms such as headache, confusion, hemiparesis, personality changes, and sometimes seizures.
Common symptoms in proportion: headache (89.6%), confusion (71.7%), hemiplegia (70.5%).2 However, symptoms are often not obvious at the beginning but progress gradually over a long time, from 3 weeks to several months. In this case, the patient was diagnosed with a subdural hematoma 2.5 months ago, but at that time there were no symptoms of the disease. It was not until 3 days before admission that the patient showed symptoms of weakness on the right side of the body, which is also the reason to detect cSDH in the patient. A similar case has also been reported, with an 83-year-old male patient suffering from a mild head injury and asymptomatic so he did not seek medical attention, 3 months later the man presented with left hemiparesis and difficulty breathing. progressed, then went to the doctor and discovered a calcified subdural hematoma in the right hemisphere.7
In 2015, a special case was reported in India, a 58-year-old male patient suffered from paralysis of the lower extremities 1 week ago. Two days before admission, the patient was urinary retention, unable to defecate. The patient had no history of trauma and other pathologies. He was diagnosed with a chronic right frontal-parietal-occipital subdural hematoma.8 In 2017, Andres M. Alvarez-Pinzon et al.9 reported a 72-year-old male patient with a history of myocardial infarction and stroke (without any complications) who was diagnosed with a subdural hematoma with rebleeding within 7 months. Two days before admission, the patient presented with personality changes, difficulty speaking, urinary incontinence, and headache.9 Thereby, neurological dysfunction can also be seen in cSDH. Patients often come to the hospital when a large hematoma is pressing on the brain parenchyma or appearance of new bleeding in the setting of a previous chronic hematoma worsening symptoms. In case the patient is in a coma, it will be difficult to intervene. On the other hand, many patients do not present with headache or focal neurological deficits, but instead have neuropsychiatric symptoms. Studies have shown that approximately 17% of cSDH patients are initially diagnosed and treated as a psychiatric illness, and up to 30% of patients exhibit only personality changes.10 One case was reported, an 82-year-old male patient was admitted to the hospital because of depression, paranoia, personality changes, was treated with sedatives for one week but did not improve, then a CT scan was indicated and discovered cSDH, which cause the midline shift to the left.11
Older people often have brain atrophy, not only losing a large number of neurons, changing mood, memory, affecting cognition, but also when the brain parenchyma shrinks, it also increases the distance from the cerebral cortex to the dura, causing the bridging veins to stretch, long-term tearing and bleeding leading to cSDH. This condition and cSDH can both manifest with personality changes, depression, and anxiety. Therefore, cSDH is easily forgotten when the patient has brain atrophy or Alzheimer’s, so, cSDH should be considered for any neurroligical changes in the elderly.
Our patient had a sizable hematoma, but the symptoms were not severe for the last 2.5 months, and the patient's brain atrophy was seen on CT of the brain. This can be explained in two ways, one is because the brain parenchyma atrophy should reduce the space-occupying effect caused by the hematoma,12 the other is because the brain of this patient has a good adaptation to the hematoma. However, when the blood mass increases rapidly, it causes hemiplegia symptoms, affecting the patient's daily activities.
In general, a brain CT scan is the imaging test chosen first for the diagnosis of cSDH, characterized by a crescent-shaped with reduced density relative to the brain parenchyma, but in case of recurrent or secondary bleeding in the brain, CT scan shows mixed homogeneity or hyperdensity.13,14 The image of the hematoma may be able to pass through the cranial joints but not the midline. MRI is the most accurate diagnostic test for cSDH, however MRI is only done when the CT scan is not clear.1,14 In some cases, angiography can be performed to determine non-traumatic causes such as ruptured aneurysms, hemangiomas in the meninges, etc.14
There are many treatments available for a chronic subdural hematoma. Regarding medical treatment, this is supportive treatment before - during and after surgery.4 Indications for surgery are made when the hematoma causes symptoms, the large hematoma presses on the midline, increases in size during follow-up... The aim of the operation is to significantly reduce the amount of hematoma, reduce symptoms, at the same time avoid recurrence and avoid complications such as bleeding, infection, convulsions, epilepsy. The popular and effective method of treatment today is surgical rinsing and blood drainage, through Burr-hole evacuation is also the method that has been applied in this patient.4 Craniotomy and twist drill craniostomy also play a role in the management.1,4
Complications of cSDH can be a recurrent hematoma, infection, new intracranial hematoma, convulsions, cerebral edema, intracranial pressure, tension pneumocephalus, and failure of the brain to expand due to cranio-cerebral disproportion.15
Unlike the acute subdural hematoma, the chronic subdural hematoma has a good prognosis if diagnosed and treated early. The mortality rate of cSDH is about 2%.16 The 1-year mortality rate after surgery in elderly patients depends on the underlying pathology.17 The prognosis of the disease depends on age, level of consciousness at initial examination and underlying medical conditions such as heart disease, kidney disease, diabetes mellitus.4
Chronic subdural hematoma is a common disease in the elderly, has a good prognosis if we recognize its signs early. This is a disease that is easy to diagnose but often overlooked due to the subjectivity of both doctors and patients. Our patient's case, despite being diagnosed and consulted before, however, the silence of the disease still made the patient come to us quite late in the condition that the subdural hematoma had increased much in size. Therefore, be on the lookout for unusual signs such as headache, confusion and hemiparesis as well as the slightest bumps especially in elderly patients, and cSDH should be considered for any neurological changes in the elderly.
None.
The authors declare no conflicts of interest.
Accepted by the ethical approval committee/Institutional Review Board of Hue University of Medicine and Pharmacy, No. 2390 / QD-DHYD, July 12, 2020.

©2021 Hoai, et al. This is an open access article distributed under the terms of the, which permits unrestricted use, distribution, and build upon your work non-commercially.